There’s a big difference between bad breath and halitosis. Bad breath is easily overcome and can literally be wiped away. While embarrassing, it’s often only temporary. Halitosis on the other hand is usually a symptom of something more sinister. If you have halitosis for real, then it won’t just go away by itself. The condition is trying to tell you something, and at Archer Dental we listen with our noses.
What is Halitosis?
Halitosis describes the regular occurrence of an unpleasant odor in the mouth. Fetor oris or ‘chronic bad breath’ is a medical condition, as opposed to occasional bad breath which could have more benign causes. Halitosis is the symptom of a more complex medical issue, and only in the best and more easily remedied scenarios is it caused by certain foods, and corresponding poor oral hygiene; more often it relates to excess alcohol or tobacco use, dry mouth, and underlying medical conditions and or related medications.
See below for a long list of medical scenarios your bad breath may be signaling.
What Causes Halitosis?
Similar to body odour, there are many causes of chronic bad breath and only one is easily treatable: poor oral hygiene. That just takes elbow grease to eradicate the odoriferous circumstances, and learning better habits helps keep it clean. Below are seven other more serious causes for chronic bad breath. Poor oral hygiene can often be cured with brushing and by using antiseptic mouthwash and other toiletries over time.
Poor Oral Hygiene can cause Halitosis
Some people have terribly unhealthy mouths, and this is mostly because they don’t put much effort into cleaning them up. They don’t brush often enough, and when they do brush their teeth, they don’t do a proper job of it. In the short term, this behaviour will likely result in some unpleasant after-dinner aromas and morning breath scenarios, but long term the daily neglect can cause more complex oral health issues.
Pungent foods such as onions and garlic and other strong-smelling flavourings can leave particles behind in your teeth and on your tongue. Fish oils and other greasy substances don’t rinse away easily, and this results in an unpleasant odor. Large quantities of sugar can also boost the bacteria count in your mouth. As the tiny organisms that live on your teeth and tongue digest the sugars, your breath turns sour. Anaerobic bacteria can produce various byproducts, including sulfur compounds which smell terrible. By and large however, this is NOT halitosis. It’s just bad breath. When food remains anywhere in the mouth, bacteria will break down the material creating a sulfur-like compound that gives off a fermented, bad-breath smell. This is the reason why Dr. Archer recommends that patients floss their teeth before they brush for best results. But this scenario is easily treated with a toothbrush and toothpaste, tooth floss and antiseptic mouthwash, and as such, this is NOT halitosis which is a medical condition that is not so easily mitigated.
Halitosis is chronic bad breath, and this medical condition is always a symptom of a greater malaise than malodorous meal choices. Repeated indulgences in smelly food combined with poor oral hygiene can create halitosis yes, but at some point, we go beyond oral health and enter into a discussion about mental health.

Dr Archer appeared on CBC The Goods to discuss Halitosis and bad breath prevention on Tuesday Jan 22nd 2018. Bad breath affects an estimated one in four people in North America. There are a number of possible causes of halitosis and the vast majority come down to inferior oral hygiene.
Dental Problems can cause Halitosis
Along with pain and discomfort, bad breath can be another way the body signals the presence of gum disease and tooth decay. Dental issues can allow bacteria to hide in cavities, or inside pockets around the gums caused by conditions such as gingivitis and periodontal disease. So chronic bad breath might be a signal its time to visit the dentist. Short-term breath freshening methods might mask the problem, but the smell always returns when core issues remain uncorrected.
Periodontitis, also generally called gum disease or periodontal disease, begins with bacterial growth in your mouth and may conclude with tooth loss due to destruction of the tissue that surrounds your teeth. Gingivitis (gum inflammation) usually precedes periodontitis (gum disease). However, it is important to know that not all gingivitis progresses to periodontitis. Read more about the treatment of Periodontal disease at Archer Dental.
Other dental causes of bad breath include poorly fitting dental appliances.
Health Problems can cause Halitosis
Besides gum disease (periodontal disease) which was discussed above, there are other health conditions that can cause halitosis. People who suffer from diabetes, cancer, kidney disease, liver disease, lung disease and respiratory tract infections, or other lesser-well-known metabolic disorders often experience chronic bad breath because of a co-symptomatic dry mouth condition. This document explores how dry mouth causes bad breath in detail below.
Diseases that affect the lungs and liver can cause halitosis in the mouth because of chemicals emitted by the body in each exhale. Your liver regulates your body’s blood sugar. If your liver can’t function properly, toxins will build up in your bloodstream and give you foul-smelling breath that takes on a sweet, musty odor. Lung cancer can (and usually will) result in bad breath. Lung cancer causes a distinct breath odor that can be measured and used in early detection of the disease. Cystic fibrosis and asthma are two other lung disorders that have a distinct odor that is associated with them (both of them smell somewhat acidic). People suffering from sinusitis, pneumonia, postnasal drip, and polyps which affects the airways may also have foul breath. Chronic bronchitis is a long-term swelling and irritation in the air passages in your lungs. The lung damage often gets worse over time, and it is usually permanent, but early signs and symptoms may include a morning cough that brings up mucus from the lungs and a bad taste or bad breath that is noticed by others.
Medications can cause Halitosis
Certain medications can cause chronic bad breath mostly because they cause dry mouth. The term dry mouth is a medical condition called xerostomia which is dry mouth resulting from reduced or absent saliva flow. Xerostomia is not a disease by itself. This is a symptom of another related medical conditions, a side effect of a radiation to the head and neck, or a side effect of a wide variety of medications. Because saliva is necessary to moisten the mouth, neutralize acids produced by plaque, and remove dead cells that accumulate on the tongue, gums, and cheek, foul odours can be produced in this region of the body simply because there wasn’t any water there to wash them away.
Other medications and drugs such as nitrates which are used in treating angina, and chemotherapy chemicals and tranquilizers such as phenothiazines (which also reduces saliva production) can increase the occurrences of mouth odor because of the breakdown and release of chemicals from the body into the patient’s breath.
Crash Diets can cause Halitosis
 Low-carb diets can cause halitosis when certain chemicals are released in the lung’s exhale as the body burns fat. This is called ketogenesis. Ketogenesis is the biochemical process through which organisms produce ketone bodies through breakdown of fatty acids and ketogenic amino acids. During the process of ketogenesis, which is when ketone bodies are formed from the breakdown of fatty acids, acetoacetate is the first ketone that’s created. Beta-hydroxybutyrate is then formed from acetoacetate. Both acetoacetate and beta-hydroxybutyrate are responsible for transporting energy from the liver to other tissues in your body. Acetone, a biproduct of acetoacetate, smells like nail polish remover and this is the odour most commonly associated with this olfactory phenomenon.
Low-carb diets can cause halitosis when certain chemicals are released in the lung’s exhale as the body burns fat. This is called ketogenesis. Ketogenesis is the biochemical process through which organisms produce ketone bodies through breakdown of fatty acids and ketogenic amino acids. During the process of ketogenesis, which is when ketone bodies are formed from the breakdown of fatty acids, acetoacetate is the first ketone that’s created. Beta-hydroxybutyrate is then formed from acetoacetate. Both acetoacetate and beta-hydroxybutyrate are responsible for transporting energy from the liver to other tissues in your body. Acetone, a biproduct of acetoacetate, smells like nail polish remover and this is the odour most commonly associated with this olfactory phenomenon.
Acetone, which is the simplest and least-used ketone body, is created spontaneously as a side product of acetoacetate. Acetone, or propanone, is the organic compound with the formula (CH₃)₂CO. It is a colorless, volatile, flammable liquid and is the simplest and smallest ketone. Acetone is miscible with water and serves as an important solvent in its own right, its most typically used for cleaning laboratories and as nail polish remover. If your breath smells like acetone, or nail polish remover, it may indicate that there are high levels of ketones in the blood. This may stem from your low carb diet, or diabetes, alcohol use, or dietary habits. If acetone is not needed for energy, it will break down and be removed from the body as waste through the breath or urine. Acetone is the cause of a characteristic fruity smell on the breath when someone is in ketosis or ketoacidosis.
Whether a person has type 1 or type 2 diabetes, an acetone-like scent in the breath can indicate diabetic ketoacidosis (DKA), a potentially life-threatening complication that needs immediate medical attention.
Acid Reflux can cause Halitosis
Chronic acid reflux, which is also known as gastroesophageal reflux disease is a medical condition. Acid reflux is the backward flow of stomach contents such as undigested food, regurgitated bile, and stomach acids into your esophagus. This can lead to tooth decay (as the acid dissolves enamel) and bad breath.
What causes acid reflux? The primary cause of this medical condition in most sufferers is a faulty or relaxed lower esophageal sphincter. The LES for short is a valve-like muscle (like a thick rubber band) that forms a barrier between your esophagus and your stomach. When the LES works appropriately, it opens when you swallow to let food enter the stomach, and then it closes tightly. A faulty LES however, remains open, and this allows acids to flow back-up and into your throat. The regurgitation of stomach contents can cause heartburn and a bitter or sour taste in your mouth. What’s more, you’re also likely to experience bad breath as a result of your symptoms. Bad breath can be controlled not only by managing your GERD, but also by making a few changes. You can read more about how everyday acids and bases affect oral health and human homeostasis.
Tonsillitis can cause Halitosis
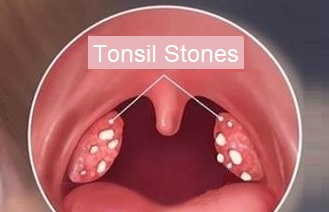 Normally your tonsils help fight infection. The small, soft, fleshy bits of tissue that reside at the back of the mouth evolved to help detect and filter bacteria and viruses that enter through the mouth. They protect the blood stream by producing white blood cells and antibodies. But tonsils are sensitive instruments that are covered with the same mucous membrane, or mucosa, that lines your mouth, nose and throat. It’s the crevices, or crypts, in your tonsils’ mucosa that may lead to smelly health problems. Inflamed tonsils get red and swollen and can cause a sore throat. Bad breath and throat irritation can also be signs of tonsillitis.
Normally your tonsils help fight infection. The small, soft, fleshy bits of tissue that reside at the back of the mouth evolved to help detect and filter bacteria and viruses that enter through the mouth. They protect the blood stream by producing white blood cells and antibodies. But tonsils are sensitive instruments that are covered with the same mucous membrane, or mucosa, that lines your mouth, nose and throat. It’s the crevices, or crypts, in your tonsils’ mucosa that may lead to smelly health problems. Inflamed tonsils get red and swollen and can cause a sore throat. Bad breath and throat irritation can also be signs of tonsillitis.
Tonsils are designed to trap bacteria; that’s their job. Unfortunately, bacteria can cause infection, and is stinky, and has a host of other characteristics that spell trouble. This is why so many children (and adults) end up getting their tonsils removed. Sometimes this bacteria becomes struck, and attracts more bacteria and other things until it eventually forms a small mass that calcifies. Tonsil stones are small calcium deposits that harden and grow on the tonsils. These are actually visible in the featured image of this blog post. The model has tonsilloliths or tonsilliths which is the medical term for this phenomenon. It’s not a serious condition, but since it is entirely composed of bacteria and other debris, it smells bad. Some people say it smells like vomit.
Smoking can cause Halitosis
If halitosis is defined as regular occurring bad breath and smokers get their mouth fouled after every cigarette, then technically smoking cigarettes all by itself causes halitosis.
Tobacco products cause their own types of mouth odor as the smoke is filled with hundreds of toxic chemicals. Additionally, tobacco smoke (and marijuana smoke) may increase the chances of gum disease which also causes bad breath. Three common bacteria are involved in gum disease. Porphyromonas gingivalis, Aggregatibacter actinomycetemcomitans, and Prevotella intermedia are all present in higher amounts in smokers than non-smokers. We could discuss prevention, and cessation but once again we would be departing the province of oral health and entering into the realm of mental health.
Fetor hepaticus – the breath of the dead
Fetor hepaticus occurs when your breath has a strong, musty smell. It’s a sign that your liver is having trouble doing its job of filtering out toxic substances, usually due to severe liver disease. As a result, sulfur substances end up in your bloodstream and can make their way to your lungs. When you exhale, these substances give your breath a distinct smell which some say is similar to the smell of rotting flesh. This is how and why you may hear fetor hepaticus referred to as the “breath of the dead.”
