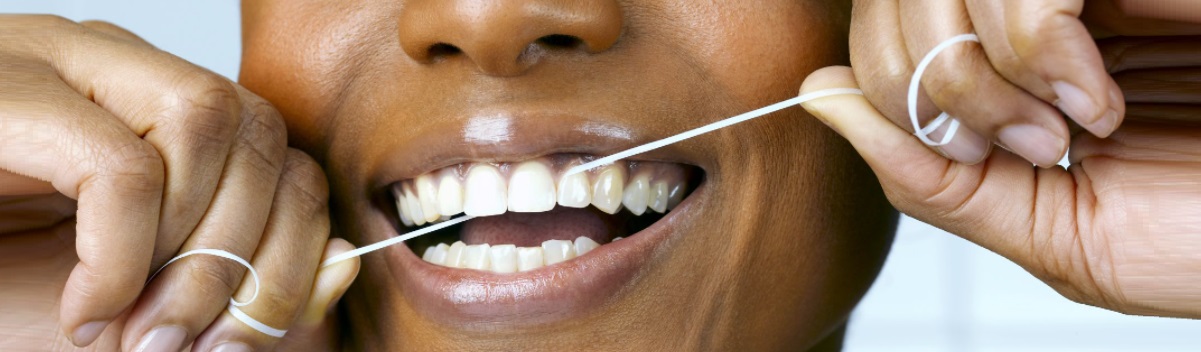
Gum Disease Treatment at Archer Dental in Toronto
What Is Periodontal Disease?
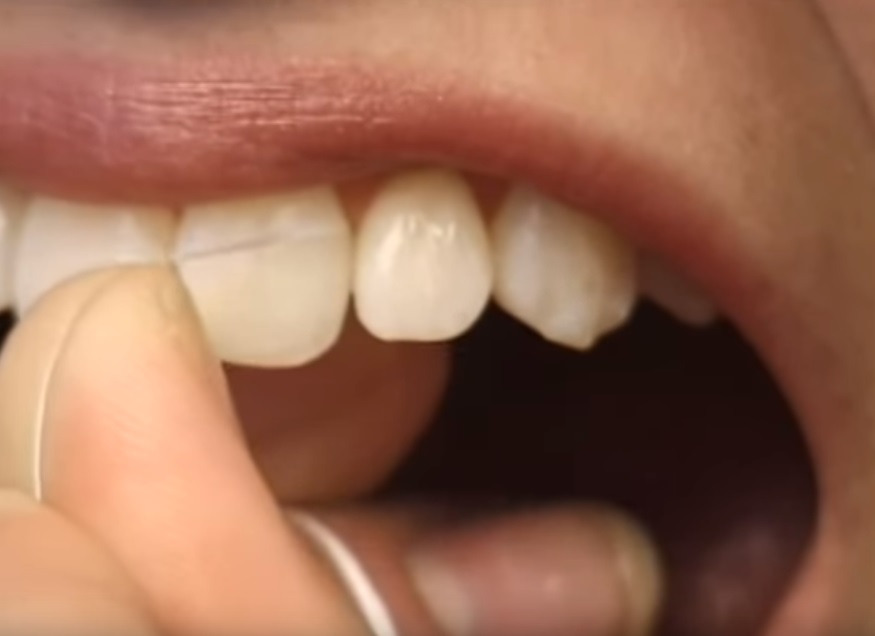
Periodontal disease, or gum disease, is a serious, progressive bacterial infection that destroys gums, ligaments, and bone supporting teeth. Caused by plaque buildup, it starts as reversible gingivitis but can lead to chronic inflammation, tooth loss, and severe damage to supporting tissues if left untreated.
This is why we brush our teeth and floss daily. Proactive morning and evening brushing and flossing rituals, combined with regular dental cleanings, are by far the best approach to preventing gum disease.
Professional teeth cleaning (scaling and root planing) is required to remove plaque and tartar below the gum line. Advanced cases may require surgical treatment. If left untreated, gum disease can destroy the tissues anchoring your teeth in place.
Symptoms of Gum Disease
Common gum disease symptoms include persistent bad breath, red, swollen, or itchy gums, and bleeding during brushing or flossing. As the infection progresses, symptoms often include receding gums, tooth sensitivity, pus along the gum line, and changes in the way teeth fit together. Early detection is critical to preventing tooth loss.
- Red, swollen, or tender gums
- Bleeding gums while brushing or flossing
- Persistent bad breath
- Receding gums (teeth appear longer)
- Loose or shifting teeth
Stages of Periodontitis
Dentists commonly describe periodontitis in four progressive stages, moving from mild to severe damage. Common clinical stages of periodontitis, as the condition progresses, would be listed as follows,
Gingivitis (early gum inflammation)
Gingivitis is what we call the common, mild form of gum disease (periodontal disease) that causes inflammation, irritation, redness, and swelling of the gingiva, the part of the gum around the base of the teeth. It’s caused by plaque buildup and, if left untreated, can advance to more serious, irreversible gum disease known as periodontitis.
Gums appear red, swollen, and may bleed when you brush or floss. They feel itchy and eating meals which require chewing feels uncomfortable and is painful afterwards.
At this early stage, only the soft tissue is affected, and the damage is usually reversible with professional cleaning and good home care.
Early periodontitis
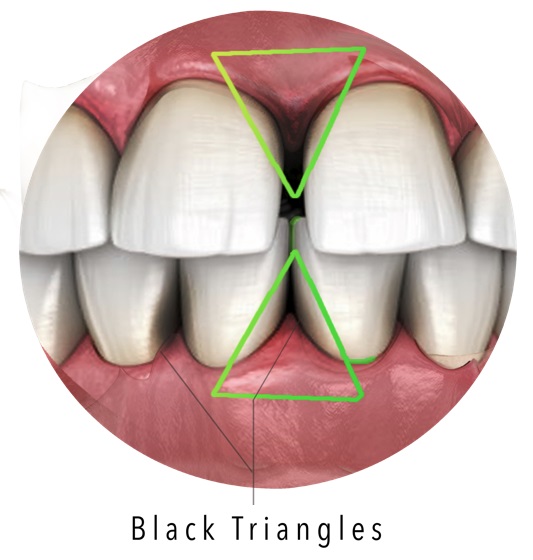
Periodontal pockets happen when gums pull away from the teeth, forming pockets that are typically 4–5 mm deep. These divots trap plaque and bacteria which can’t be removed by brushing alone. This is when the condition starts to cause bone loss.
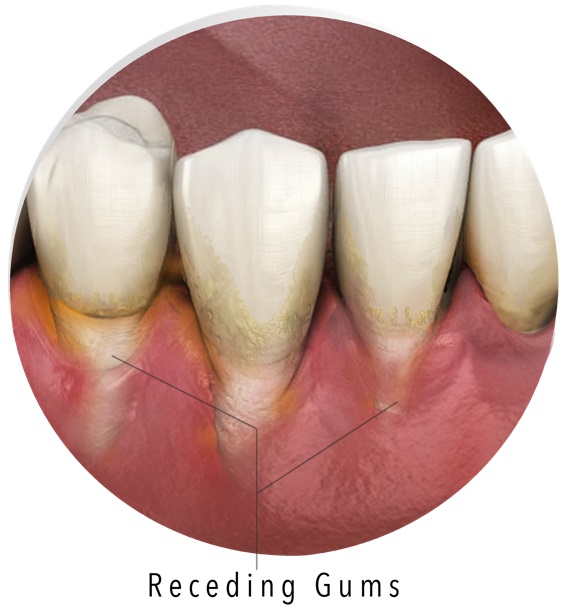
Gum recession is when your gum tissue pulls away from your teeth, exposing the roots underneath. It’s caused by a number of factors, but is a sign of advancing gingivitis.
Physical symptoms at this stage are not easily detected but can be smelled. Sufferers can feel their itchy gums and those around them may notice their persistent bad breath (halitosis) because of the the bacteria thriving in the pockets between their teeth and gums..
Moderate periodontitis
In moderate periodontitis, the infection has moved beyond early inflammation and is now starting to damage the bone and support structures that hold your teeth in place.
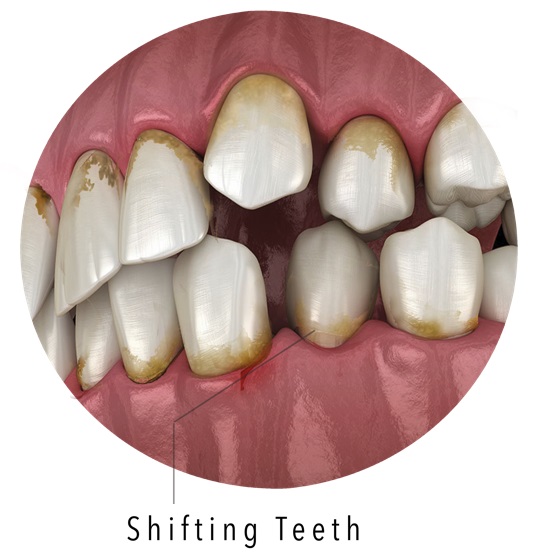
As the pockets around your teeth get deeper and more difficult to clean, X‑rays show clearer areas of bone loss, and you may notice that some teeth feel a bit loose, tender when you bite, or more sensitive to hot and cold.
As the disease progresses, the gums often pull back further from the teeth, making teeth look longer and exposing more root surface. The ongoing bacterial infection now causes persistent bad breath and even a bad taste in your mouth. You feel discomfort or dull pain when chewing, especially on certain teeth. These signs usually mean the disease is no longer in the early stage and should be treated promptly to prevent more serious damage or tooth loss.
Advanced periodontitis
In advanced periodontitis, the supporting structures around your teeth have been badly damaged, and the disease is no longer just a gum problem, The disease affects the bone and how your teeth function. Deep periodontal pockets form around the teeth and are very difficult to keep clean, so bacteria and inflammation stay trapped under the gums.
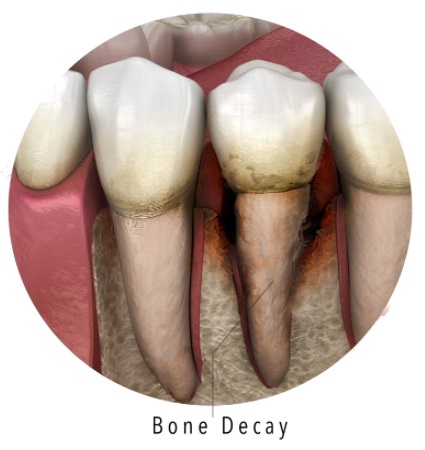
At this point, there is significant bone loss, gums have pulled back noticeably, teeth may look longer, and several teeth can feel loose or start to shift out of their normal positions. Chewing can become uncomfortable or even painful, especially on certain teeth that are taking more force because the bite is no longer even.
If advanced periodontitis is not treated, the ongoing infection can lead to painful gum abscesses (pockets of pus), further destruction of bone, and major changes in your bite and smile. Teeth may drift, flare out, or create gaps, making it harder to chew and clean properly. Eventually, some teeth may become so loose that they cannot be saved and need to be removed. In many cases, this stage requires more complex treatment such as extractions, gum or bone grafting, or replacement options like bridges, dentures, or dental implants to restore function and appearance.
How Archer Dental Treats Gum Disease (scaling and root planing, hygiene therapy, laser therapy, referrals)
Led by Dr. Natalie Archer, our team of friendly experienced dentists and dental hygienists treats gum disease with a gentle, step‑by‑step approach tailored to your condition. In a professional dental cleaning, our hygiene therapists start with scaling and root planing to remove plaque and tartar below the gum line, then use ongoing hygiene therapy to help your gums heal and stay healthy. When appropriate, we add laser therapy to disinfect deep pockets more comfortably and precisely. For complex or advanced cases, we coordinate referrals to trusted periodontal specialists, so patients receive the right level of care while we’ll remain your dental partners for regular, ongoing maintenance.
Why Choose Archer Dental for Gum Disease Treatment?
Archer Dental blends comprehensive periodontal care with a preventative, comfort‑focused approach delivered across multiple Toronto locations. Our methods and technology, and our philosophy is aligned with patients who need ongoing management of gingivitis and periodontitis rather than one‑off “fixes.”
Comprehensive gum disease care
Archer Dental treats all stages of gum disease, from early gingivitis to advanced periodontitis, rather than limiting care to routine cleanings. During teeth cleaning with oral exams, clinicians specifically screen for gum disease and oral cancer, so periodontal problems are caught and managed early. Their services include non‑surgical periodontal therapy in‑house and access to surgical options via specialists when needed, giving patients a full care continuum under one umbrella.
Specialized hygiene therapy model
Archer Dental uses “hygiene therapists” (dental hygienists) who go beyond standard cleanings to deliver structured hygiene therapy aimed at treating and preventing periodontal disease. These clinicians perform periodontal charting, debridement (scaling and root planing), prophylaxis, and periodontal maintenance tailored to each patient’s disease stage. They also educate patients, monitor gums over time, and provide personalized treatment plans that focus on behavior change and home care, which is critical for long‑term control of gum disease.
Periodontics
Periodontics includes the placement of dental implants beneath the gum line as part of the process to replace missing teeth. Once the gums have healed, a tooth replacement can be added, and replacing missing teeth is always the best outcome.
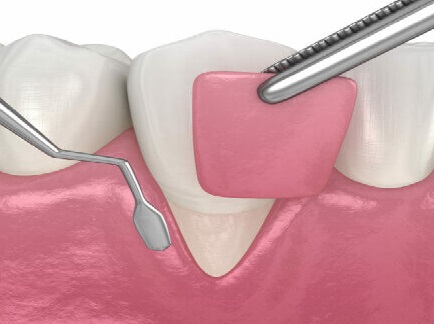
Soft tissue periodontics involves surgical procedures, primarily soft tissue grafting, to treat gum recession, reduce tooth sensitivity, and improve the aesthetics of the smile. These procedures, including free gingival and connective tissue grafts, use donor tissue which is often collected from the roof of the patient’s mouth. This tissue is used to cover exposed roots, thicken thin gums, and protect against further bone loss.
Technology, monitoring, and prevention
Hygiene therapists at Archer Dental use X‑rays, ultrasonic scalers, and other modern tools to diagnose and treat gum problems accurately. They maintain detailed historical records and periodic gum assessments, allowing them to track disease progression or healing over multiple visits.
Routine oral exams at the practice integrate cavity checks, gum‑health evaluations, and oral cancer screening so that periodontal disease is managed within a broader preventive‑care framework.
Cost of Gum Disease Treatment
Gum disease treatment costs at Archer Dental, based on Ontario Dental Association (ODA) fee guides, range from $66 for 15 minutes of scaling up to $264 for a full hour of hygiene therapy. More advanced periodontal procedures, such as gum grafts, can cost approximately $1,950 per application site.
Scaling/Root Planing: $66 (15 min) – $264 (60 min)
Hygiene Therapy (Comprehensive): $264+
Gum Grafting: ~$1,950 per site
Dental Bone Graft: ~$2,215
Comprehensive Exam (New Patient): $96–$191
Digital X-Rays: $43+
Gum disease treatment factors which affect cost:
Treatment costs are based on the severity of patient’s condition. Costs vary based on the extent of plaque, tartar, and bacteria removal required. Treatment may include specialized hygiene therapy, scaling, or in severe cases, surgical interventions. Archer Dental provides written estimates and reviews insurance coverage before beginning treatment.
Can You Reverse Gum Disease?
Yes, early-stage gum disease (gingivitis) is fully reversible with professional dental care and improved daily oral hygiene. Advanced gum disease (periodontitis) however, causes permanent damage to bone and tissue that cannot be reversed, although it can be managed and halted through treatments like deep cleaning.
Gum Disease Treatment is available at Archer Dental clinics
Each clinic has teams of dental professionals; the resident dentist, dental hygienist and dental assistants are highly experienced at cleaning teeth and taking steps to remedy periodontal disease. The practice happens regularly at Archer Dental Baby Point, and in the downtown core at Archer Dental Rosedale and at Archer Dental Little Italy. The same level of expertise and gentle care is provided at all three clinics.
At each Archer Dental clinic, dental hygienists, and dental assistants clean teeth and experienced dentists diagnose the severity of gum disease using modern equipment and techniques. Each location offers Archer Dental’s uniform commitment to patient comfort and affordability.
Common Questions About Gum Disease
What Causes Gum Disease?
Plaque Build-up: Bacteria, mucus, and food particles form plaque that, if not removed, hardens into tartar (calculus). Poor Hygiene: Inadequate brushing and flossing. Risk Factors: Smoking, diabetes, hormonal changes (pregnancy, menopause), and genetics.
What is the Difference Between Gingivitis and Periodontitis?
Gingivitis is the initial, mild stage of Periodontitis, characterized by inflammation at the gum line. It is reversible with proper home care and professional cleanings. Periodontitis itself is the advanced stage where plaque spreads below the gum line, destroying the bone and ligament supporting the tooth. This damage cannot be reversed and requires professional treatment.
Can Gum Disease Be Completely Cured?
Gingivitis can be cured (reversed), but periodontitis however cannot be fully cured once bone loss occurs; it can only be managed to stop further damage.
Is Gum Disease Contagious?
While not contagious like a cold, the bacteria that cause it can be passed through saliva, such as sharing utensils or kissing.
Book a Gum Disease Assessment in Toronto
Contact Archer Dental to book a teeth cleaning and new patient exam.