Signs of Gum Disease
Periodontitis, known more commonly as gum disease, is a serious infection that damages the soft tissue of the mouth. The condition is preventable and usually the result of poor oral hygiene. Plaque and tartar build-up can destroy the bone that supports teeth. Treating gum disease requires deep cleaning teeth and maintaining proper oral hygiene. Without proper treatment, periodontitis can cause teeth to loosen in the patient’s mouth and this leads to tooth loss.
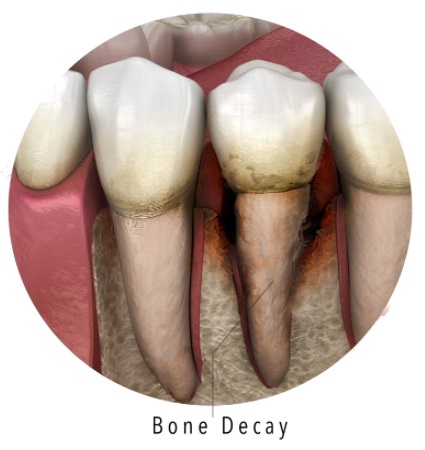
A recent study by the Canadian Dental Association (CDA) concluded that over 20% of Canadian adults, or one in every five people have experienced or are currently battling periodontal disease.
Gum disease can be defeated with good oral hygiene. Once infected, sufferers can fast track recovery with a professional teeth cleaning service. Regular brushing and daily flossing and getting regular dental checkups are the best ways to keep teeth clean and maintain optimal oral health. Proper oral hygiene is the successful treatment for periodontitis, and greatly reduces patients’ chances of developing it in the first place. Hygiene therapists at Archer Dental offer comprehensive oral health care treatment programs.
List Common Gum Disease Symptoms
Healthy gingival tissue is dense and pink and contains a good supply of blood vessels beneath a moist surface, otherwise known as a mucous membrane. The gingival tissue connects with the rest of the mouth lining but is pink instead of shiny red. Healthy gums are firm, pink and fit snugly around teeth. Signs you might have periodontitis start with,
- Bloody teeth that bleed after brushing and flossing
- Bad breath is a sign of dirty teeth and decay
- Discomfort – Itchy gums that feel like they need scratching
- Receding gums and long teeth
- Abscesses and infections caused by loose gums
- Black triangles in smile
- Shifting teeth and changing bite patterns
As gum disease runs its course, and bacteria eats bones, teeth shift and sufferers may notice changes in their bite and eating anything can be torturous. This blog post will chart the progress of the disease by asking common problems about the symptoms.
Are Bleeding Teeth a sign of Gum Disease?
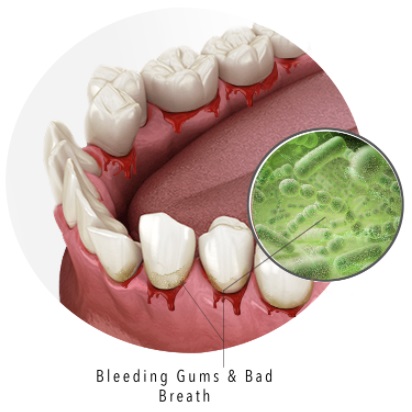
Yes. Bleeding is a common symptom of early stage gum disease; teeth look and feel relatively healthy, but patients notice occasional bleeding when eating certain foods such as apples and biscuits. Everyone is different, but generally speaking, patients’ gums will mostly seem normal, with no swelling or irritation, but the blood smear is a sign of trouble to come.
Mild bleeding is considered normal from time to time, even in healthy gums, but when patients experience it more frequently, they’d be well advised to step up their own oral hygiene routine and check with their dentists to see whether they’re experiencing the first stages of gum disease.
Archer Dental blog has already discussed all the particulars related to Bleeding Gums when Brushing and Flossing.
Bleeding gums can also point to other health problems. Occasional bleeding of the gums can be caused by brushing teeth too vigorously or wearing dentures that don’t fit correctly. Frequent gum bleeding indicates serious problems.
Is Bad Breath a Sign of Gum Disease?
Persistent bad breath and patients’ experiencing a bad taste in their mouth may be a warning sign of gum disease. Periodontal disease is caused by the buildup of plaque on teeth. Odorous bacteria toxins are also produced. Bad breath is also called halitosis, and can be embarrassing and in some cases may even cause anxiety. This is why convenience store shelves are overflowing with gum, mints, mouthwashes designed to fight bad breath. But many of these products are only temporary measures because they don’t address the underlying cause of the problem.
Dr. Natalie Archer went on CBC The Goods to discuss strategies of how to defeat halitosis.
Chronic bad breath can be caused by oral bacteria that emit sulfur-producing compounds into the oral environment. These bacteria live within the plaque that accumulates on the teeth and gums, and is the first stage of gum disease.
Are Receding Gums a Sign of Periodontal Disease?
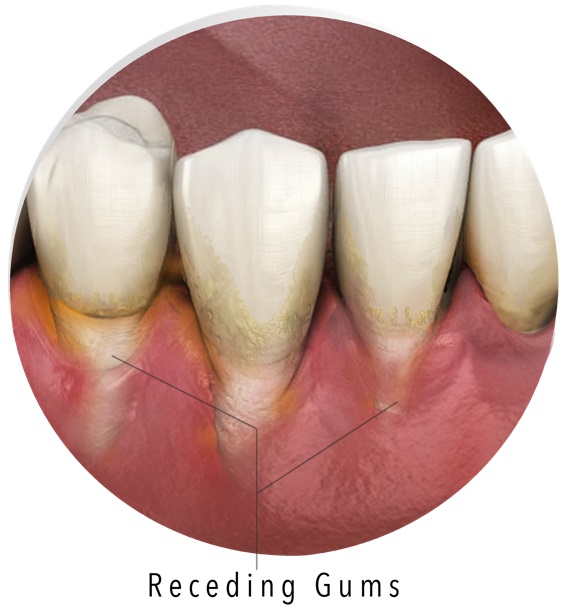
Periodontal disease can certainly cause gum recession, a process in which the gum tissue that surrounds the teeth wears away, or pulls back, exposing more of the tooth, or the tooth’s root. The acid created by harmful bacteria destroys the supporting tissue and bones, thus making the teeth look longer and smiles appear more “toothy.” Additionally, plaque around patients’ teeth starts to harden into a tougher, more damaging material called calculus or tartar, and this causes the damage to accelerate.
When gum recession occurs, “pockets,” or gaps, form between the teeth and gum line which makes it easy for disease-causing bacteria to accumulate. The toxins produced by bacteria produce an acid capable of destroying a tooth’s outer barrier, and this results in tooth decay, gingivitis, and halitosis.
At this stage, bone structures anchoring teeth to the patients’ jaws may be beginning to weaken, and patients should see a dentist quickly to reduce the risk of tooth loss. In the early stages of periodontitis, a thorough cleaning and a strong course of antibiotics is usually enough to stop the disease from progressing, and can even start to repair the damage. However, the longer this condition is left untreated, the harder it is to cure.
Are Mouth Infections a Sign of Gum Disease?
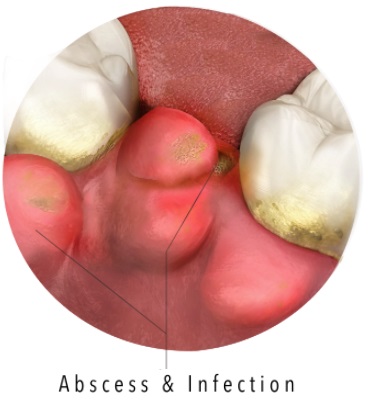
An abscess can occur with serious gum disease (periodontitis), which causes the gums to pull away from the teeth. This leaves pockets where bacteria can grow. If an excessive amount of tartar has formed, or if food gets stuck in the pockets, it forms pus. If this fluid can’t drain away, the pus builds-up and forms an abscess. Pus oozing from between the teeth is definitely a sign of periodontal disease. The pus is a result of the body trying to fight the bacterial infection.
The infection supercharges disease-causing bacteria which can cause redness, and swollen gums that ooze pus, sensitivity, loosening of teeth, painful chewing, severe bad breath, and bone loss.
The same bacteria gradually eats away at the underlying jawbone and loosens the periodontal ligaments that connect the tooth to the bone.
Are Black Triangles Between Teeth a Sign of Gum Disease
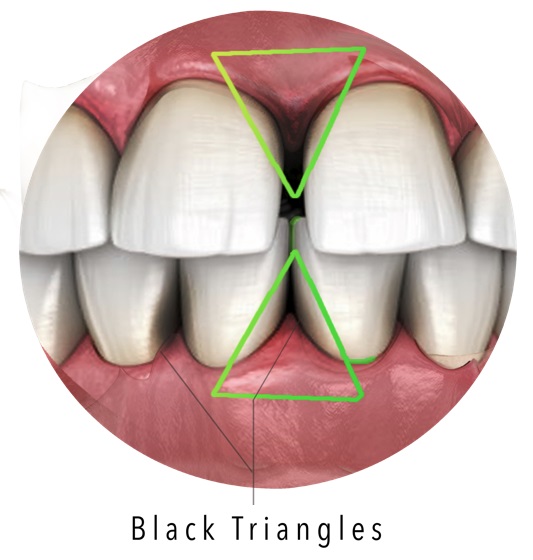
Yes, shadows between teeth are a sign of gum disease. As gum disease advances, tissue shrinks, bone decays and teeth become loose and that’s when gaps appear in smiles. The human jawbone, and the proper-working of the muscles and cartilage that comprise the jaw is preserved through the pressure and stimulus of chewing. As the bone tissue gets destroyed, teeth that were once firmly attached to the jawbone become loose and are more easily shifted into new positions.
To remove the black triangles, it’s essential to halt the progression of the infection before the gums and jaw bone have been affected. The empty spaces used to be filled with gum tissue known as papilla. When these tissues recede or are lost, the empty spaces appear as black triangles.
Advanced periodontitis may require invasive dental surgery to clear away the disease, and even then the damage may have gone too far to be remedied.
What are the Symptoms of Advanced Periodontitis?
With advanced gum disease or periodontitis, patients will notice pain when chewing and experience different bites due to different tooth alignments. They could have receding gums and dark pockets between their teeth. They might have loose or sensitive teeth and sores inside their mouths. Their friends and family will notice their persistent bad breath.
With advanced periodontitis, patient’s gums will be visibly shrunken and large portions of their teeth will be exposed. Many teeth will be loose, even ones which look healthy, because the infection is now attacking the patient’s jawbone. Without treatment, the patient will almost certainly lose the tooth.
Is a Changing Bite a Sign of Gum Disease?
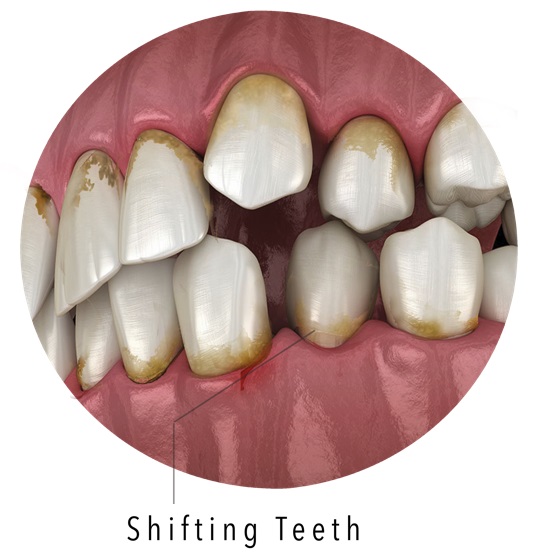
Loose teeth indicate rapidly progressing gum disease. As the bone tissue gets destroyed, teeth that were once firmly attached to the jawbone become loose and are more easily shifted into new positions.
If patients have a missing tooth, the surrounding teeth will naturally move because of the extra space that’s available. Depending on how much teeth shifting has already occurred, you may need a dental professional to straighten your smile. The fix is going to depend on the cause and severity of the issue
Essentially periodontal disease all boils down to the bacteria. If plaque and tartar are not regularly removed using good daily flossing and brushing habits, as well as regular professional teeth cleanings, then periodontal disease will almost certainly occur. Smoking is the most significant risk factor and can make periodontal disease treatment less effective. Other factors that increase one’s risk for periodontal disease include diabetes, medications that reduce the natural flow of saliva, genetics, hormonal changes, and certain illnesses like AIDS.
Adopting healthy habits is the key to defeating periodontitis in the long term. If the movement is being caused by tooth decay or gum disease, patients will have to undergo treatment. If patients’ teeth have shifted a little too much, orthodontics like braces or Invisalign will get you sorted out
Teeth cleaning is called Hygiene Therapy at Archer Dental and is administered by Archer Dental’s hygiene therapists who manually remove plaque from teeth using hand scrapers and sonic power washers. While there’s no curing periodontitis, there are ways to stop the progress of the disease and help mitigate the discomfort caused by having this condition.

