On Wednesday, March 25th Rachael D’Amore telephoned Dr Natalie Archer DDS to ask about dentistry in the Age of Coronovirus. Like so many other Canadians, dentists have also had to adjust to a new business reality amid the pandemic that has now closed most dental clinics in Ontario. Yet we search for ways to be productive and helpful.
What exactly does ‘Emergency Care Only’ mean for dentists and patients?
Provinces and local governments have imposed increasingly tight controls to try and curtail the spread of COVID-19 and they ultimately encourage as many people as possible to stay home. Quebec and Ontario, for example, have ordered all non-essential businesses to close, but the rule vary and are slightly different in each jurisdiction.
Those deemed essential are somewhat obvious; health-care workers, first responders, suppliers of critical goods like food and medicine, and utility workers are encouraged to go to work and help save lives and keep society functioning. So where does that leave dentists?
Ontario, Quebec and British Columbia have ordered a pause on “non-essential” dental services like teeth cleaning, teeth whitening obviously and other cosmetic procedures. Only emergency care, like facial trauma or pain that can’t be managed with antibiotics or over-the-counter medications, can be performed. Dentists in other provinces, like Manitoba, have taken it upon themselves to put similar measures in place for their residents. But even then, there are risks.
“We have to set a high bar for emergencies in dentistry because it’s such high risk. We’re one of the most at risk in this,” said Dr Natalie Archer. “We’re still learning about the virus, but we definitely know it’s spread through things like mucus and saliva. These are things that dentists are intimately connected with… There’s no social distancing when it comes to treating patients in dentistry.”
The respiratory virus is spread mainly from person-to-person, either by close contact or “respiratory droplets.” So when an infected person coughs or sneezes, if the resulting droplets end up in the mouths or noses of people nearby, either by inhalation or contact, those people can become infected.
In health care, increased risk comes with increased protocols. In Ontario for example the Royal College of Dental Surgeons (RCDSO) has clamped down on what constitutes an emergency dental situation and has issued directives on screening procedures as well as which tools to use when. They stipulate that only emergency care, like facial trauma or pain that can’t be managed with antibiotics or over-the-counter medications, can be performed.
What is an essential service?
Rachael D’Amore’s reporting also shared some interesting data. Between 2017 and 2018 there were over 93,000 dental visits at the University of Toronto’s Faculty of Dentistry, which allow students to treat patients. Of those, 4,000 were considered emergency dental visits. So based on that ratio you can see there’s a demand that will not be abated by stay-at-home social directives. Some dentistry is essential.
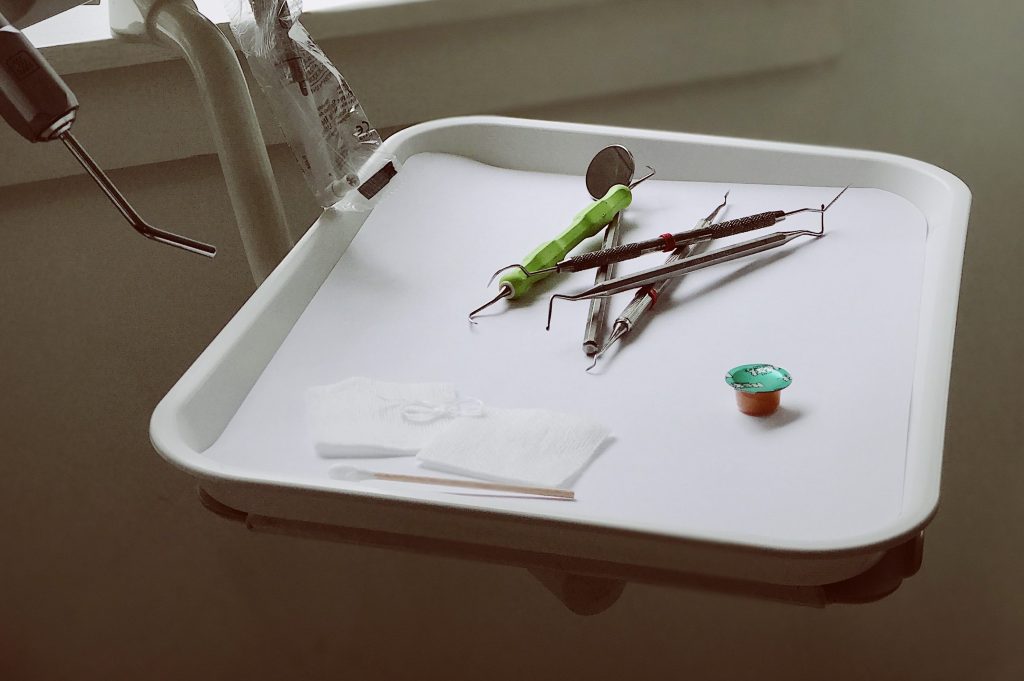
Readers should know that infection control in dentistry is already at a high professional standard. Sterilizers are tested every day, there are chemical indicators that show that everything’s been sterilized properly, there’s tracking of every instrument, everyone’s wearing the proper PPE (personal protective equipment),” he said. Infection control protocol standards for dentistry are incredibly high. But that efficiency doesn’t negate the fact that dentists need to be in close contact with patients to do the job.

Sterilization of equipment happens routinely in autoclave at Archer Dental Rosedale
“The primary thing is to keep people safe and healthy but you also really have to keep them out of hospitals unless they absolutely need to be there — the system’s already facing a burden.”
Archer Dental Emergency Dental Service in Toronto
Archer Dental patients can set up phone-call screening and counseling or FaceTime a dentist for certain inquiries. We offer emergency dental services such as it abides with RCDSO’s new required safety practices, but we can also provide some level of comfort to patients locked away at home who need advice, said Archer. Patients are encouraged to call their office and their calls will be received and scheduled accordingly.
“I think it makes patients realize what is a real emergency right now,” Dr Archer said. “As a dentist, we have to assume that everybody we come into contact with has COVID-19. So that’s the level of care we take when we decide what’s an emergency.”
The article ends with Dr Archer’s quote; “There’s a very good chance that you’re not going to get into a dental office for a check-up for quite some time, so this is the best opportunity to take care of ourselves from a preventative side,” Natalie said. “People always tell me they don’t have time to floss. Guess what? You’ve got time. You’ve got more time than you know what to do with. Now’s the time to floss.”