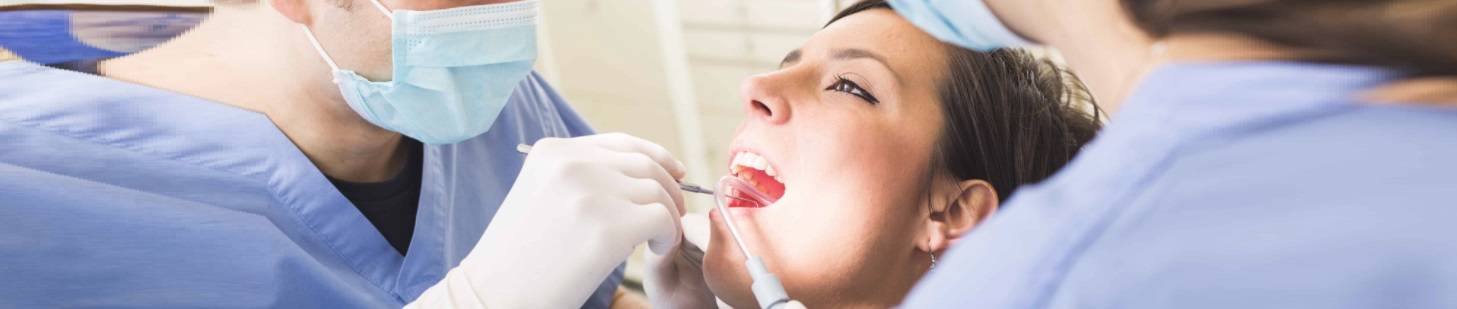
A root canal is a last chance dental treatment that’s done to save a decayed or infected tooth, as an alternative to extraction. The word root canal originates from the Edwin Maynard’s pioneering dental procedure, first attempted in 1838. That operation was done with a watch spring. Gutta percha was adopted to fill dental root canals as early as 1847, a material (now synthetic) which dentists still use today. To receive a root canal is to have the inner core of your tooth cleaned of decay and then resealed with a biologically inert, resilient, electrically nonconductive, thermoplastic filling.
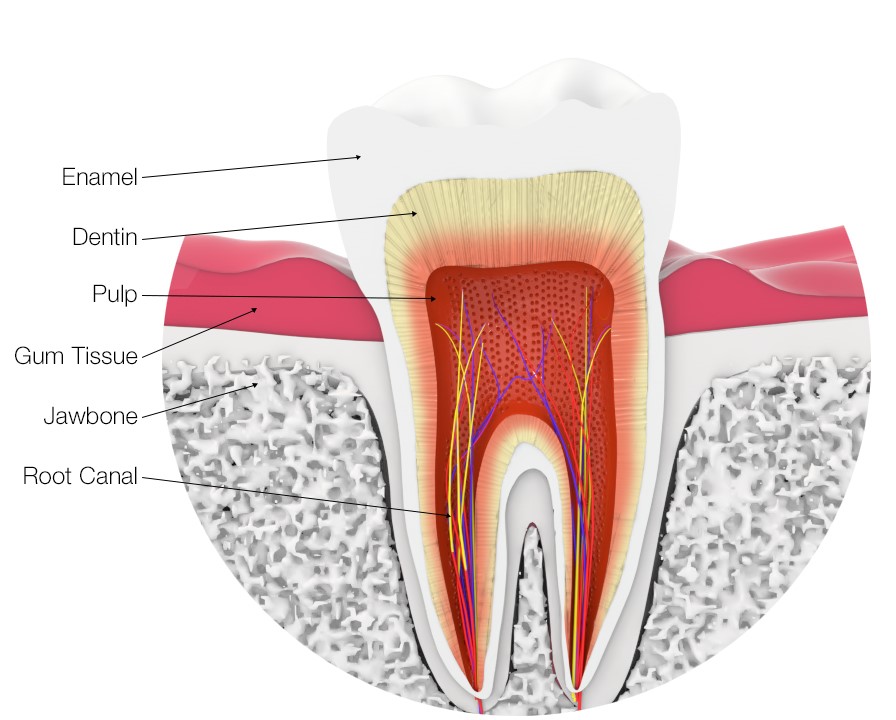

- How long does a root canal take?
- Does root canal treatment hurt?
- How much does a root canal cost?
- What causes a root canal?
- How do I know I need a root canal?
- How long does a root canal last?
- How is a root canal done?
- What to expect after a root canal?
How long does a root canal take?
At Archer Dental, a typical root canal procedure (without any complications) takes over an hour and could stretch to ninety minutes for the entire appointment. More complex procedures may take even longer. We recommend you bring your own listening device, or you can watch Netflix during your surgery. Yes, this is possible.
Does root canal treatment hurt?
‘Freezing’, what we call modern anesthetics, makes root canal procedures relatively painless. There could be some discomfort during the needling but even that is reduced with topical anesthesia. After the freezing wears off, hours later, there may be some discomfort for a day or two, which can normally be controlled with over-the-counter painkillers. Occasionally your dentist may prescribe antibiotics to treat any lingering infection.
How much does a root canal cost?
Root Canal Treatment costs between $540 and $1250 dollars in Toronto. Also referred to as endodontic therapy, a root canal is sometimes the only option to retain a tooth that has suffered severe damage or has become infected. Front and back teeth have a varying number of roots. Root canals on incisors (front teeth) usually cost less because they only have one root, while the same procedure on molars (back teeth) will invariably cost more because these teeth have three or more roots. Teeth that are calcified i.e. older adults may be more costly. Radiographs help determine the difficulty of the root canal. At Archer Dental we also work with independent endodontists to assist with the most complex cases. Read more about Oral Surgery at Archer Dental.
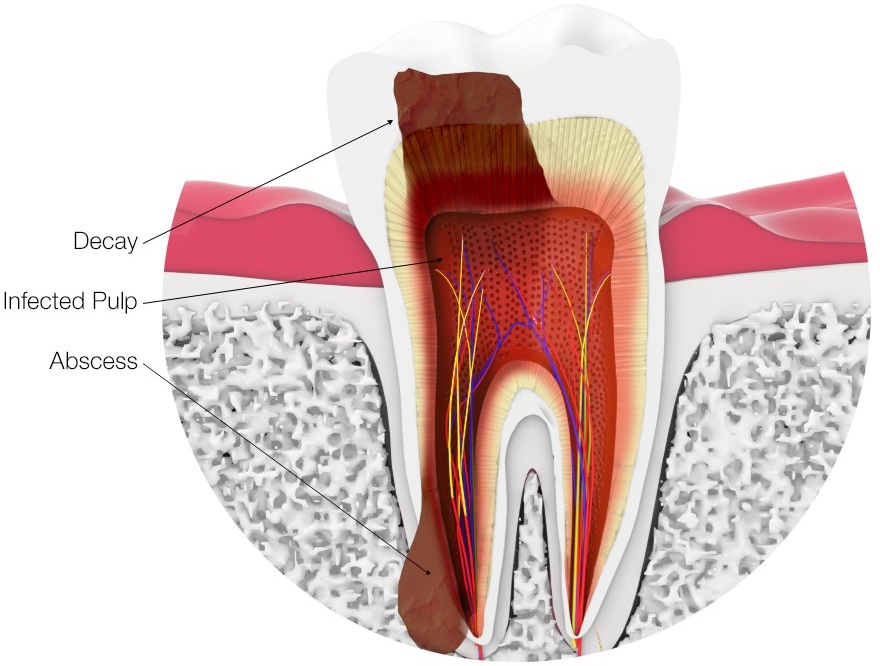

What causes a root canal?
Neglect causes root canals. It takes some time for a tooth to decay to the point where endodontic therapy is recommended. Warning signs of tooth decay, such as cavities, will occur and fester for months or even years before it becomes necessary to pursue such intensive treatment. Yet there are some common situations that can make a root canal procedure more likely. Failure to brush or floss regularly allows the continued development of bacterial biofilm that turns to plaque. Flossing helps clean hard-to-reach areas between teeth. Not visiting the dentist regularly means there is no supervision and dental ailments get exponentially worse over time.
How do I know I need a root canal?
The best way to determine if you need a root canal is to get an expert opinion from a dentist. Set up an appointment for a dental examination. When seeking out infections underneath patients’ teeth, the dentist will need to take X-rays to visualize what’s happening. Dentists will diagnose and prescribe the best treatment based on the medical imaging. The most common symptoms of pain that result in a root canal treatment are:
- Discomfort and ‘shooting’ pain while chewing or biting
- Feeling and seeing pimples on gums near the troubled tooth
- A cracked or chipped tooth
- Swollen or tender gums
- Lingering sensitivity to hot or cold foods, even after more severe pain has subsided.
How long does a root canal last?
Archer Dental has very good results with endodontic therapy. The vast majority of our patients report no pain after the procedure and only minimal discomfort during surgery. The restored tooth should remain maintenance free for years and infection free for decades.
How is a root canal done?
Archer Dental’s Root Canal Procedure has evolved over time with new medication and instrumentation and our own experience; we’ve performed countless endodontic surgeries at all three locations in the many years we’ve been in business. If you’re reading this and wondering exactly what happens, let us guide you through the proceedings.
Step 1: Topical & local anesthesia is applied
Topical anesthesia is administered by the dentist to the gums around the problem tooth before needles to inject local anesthesia are used to numb the tooth and surrounding area. The attending dentist will then wait the required amount of time until the area is completely numb before beginning treatment.
Step 2: Dental dam to protect patient’s mouth
A thin sheet of latex, a rubbery insulative material is applied to the patient’s mouth by the dentist or dental assistant. This dental dam as it’s called allows the dentist to focus on the one specific tooth receiving treatment. The sheet effectively eclipses the other surrounding teeth and provides a sterile environment that reduces the risk of injury or infection by the natural bacteria present in a patient’s mouth.
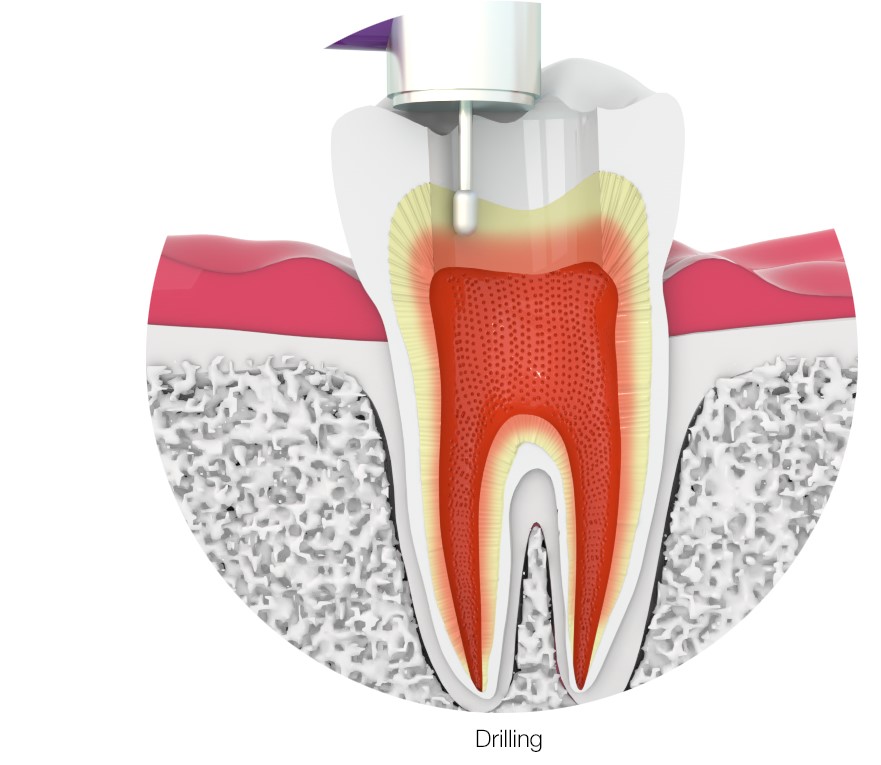

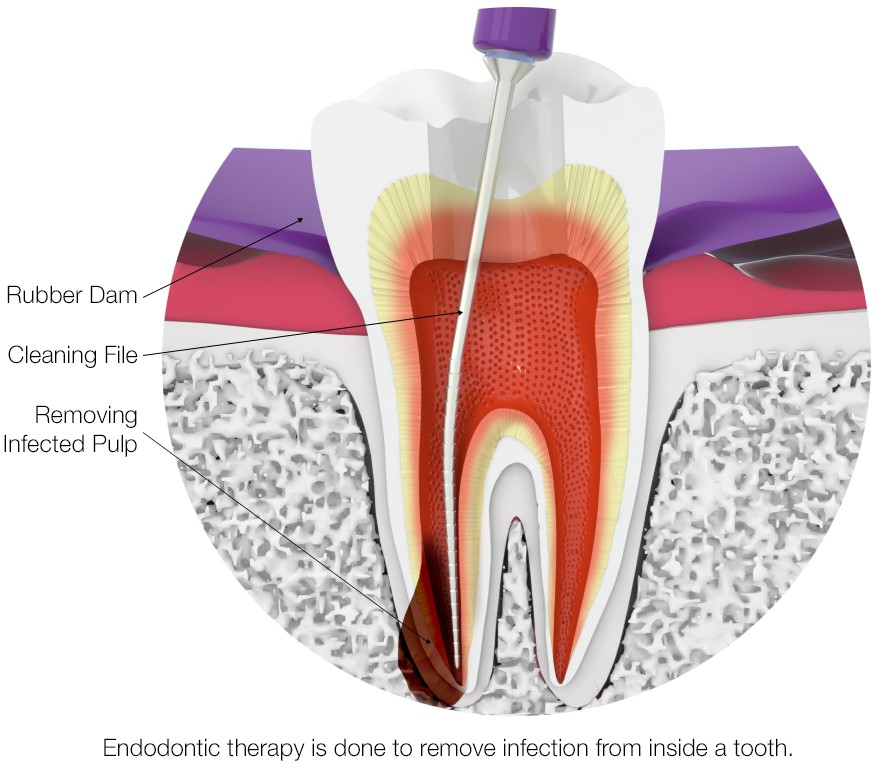

Step 3: Drilling and removing decayed matter
To access and clear away the infection deep in the tooth, an access hole must drilled in the surface. Depending on the location of the tooth, this opening may be along the biting surface or in the back of the tooth. Very small and specialized root canal instruments, called files, are used to remove the infected pulp tissue, and the nerves, and to shape the canals. At this point, the tooth is desensitized to pain (as the nerves are removed). The most important part of this third step is to disinfect the insides of the tooth, or the root canals.
Step 4: Remove tissue and nerves
Special root canal tools are used to remove the dead pulp tissue and nerves. At this point, the affected tooth will no longer be able to feel pain. It’s important to note, the nerves are not “killed” during endodontic treatment, but rather i the inflamed or infected pulp tissue, containing nerves and blood vessels, is removed from the pulp chamber of a tooth to prevent the further spread of infection and decay.
Step 5: Disinfecting the affectedtooth
After the tooth is cleaned and shaped, the disinfected canals are filled with a biocompatible thermoplastic filling material called gutta-percha (originally derived from a plant in Malaysia). This material is set in place by an adhesive cement sealer; which is very important to keep the tooth from becoming re-infected later.
Step 6: Insert flexible root canal tools
Flexible root canal tools are inserted into the canals of the tooth to help shape an area for the filling and sealer. A final cleaning is performed at this point to remove any remaining debris.
Step 7: Apply synthetic filling material
A rubber-like, thermoplastic filling material called gutta-percha (originally derived from a plant in Malaysia) is applied into the root canals and set in place by an adhesive cement sealer. The sealer is very important to keep the tooth from once again becoming infected
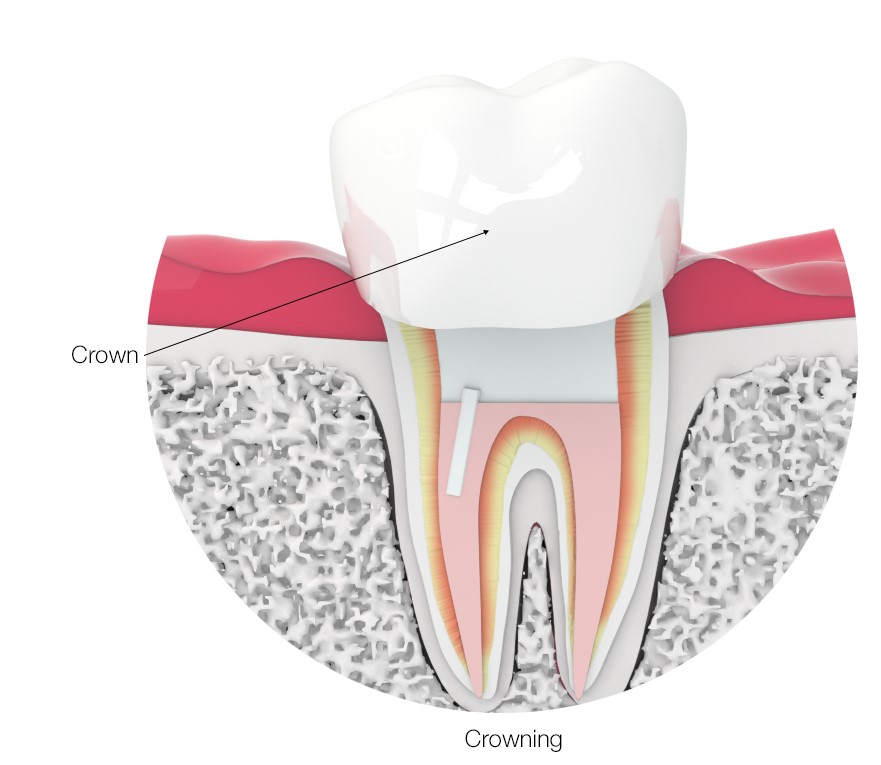
Step 8: Restoring the tooth
Once the life source or the nerve of the tooth has been removed, the tooth is fragile and more prone to crack and fracture which may result in the tooth requiring a post and crown. The need for a crown depends on the location of the tooth in the patient’s mouth. The teeth they depend on for biting and chewing generally require crowns whereas front teeth can often be restored with a filling.
Depending on the structure of the affected tooth, a post may be inserted into the root canal during the filling process to help hold the temporary or permanent filling in place. If you receive a temporary filling, it is very important to come back for a permanent filling or crown to reduce the risk of infection down the road.
In most cases, an antibiotic will be prescribed to treat any remaining infection. It is common to feel some minor pain and discomfort after the procedure, but it should only last a couple of days.

What to expect after a root canal?
Following root canal treatment it’s normal to experience some discomfort and minor swelling. This pain should be easily managed with Advil or Tylenol. If patients are unsure that what they’re feeling is normal, please call us – we are here to help!